
Understanding the Ebola Outbreak
Oct 22, 2014
Editor's Note: The forthcoming update to AIR's pandemic model will cover emerging infectious diseases, including coronaviruses and filoviruses such as Marburg and Ebola. The Ebola outbreak is currently showing no signs of slowing, and projections show the possibility that hundreds of thousands of people could be infected by early next year, mainly in West Africa. The potential for sustained and widespread infection across multiple continents remains low. AIR disease modeling experts share their insights in this article.
Accelerating Progression
The current Ebola outbreak, in West Africa, is the most severe on record. It has killed more people than all previously recorded outbreaks combined since the virus was discovered in 1976. The current outbreak is believed to have started in Gueckedou, Guinea, in December 2013. On March 25, 2014, the disease was identified and reported by the World Health Organization (WHO). By August, cases had spread to Liberia, Sierra Leone, and Nigeria. WHO designated the event as a Public Health Emergency of International Concern. The numbers of confirmed, probable, and suspected cases and deaths to date (as of October 17, 2014) are shown in Table 1; the actual counts are likely to be much higher due to significant under-reporting.
| Number of cases | 9,216 |
Number of deaths | 4,555 |
| Countries affected | Guinea, Liberia, and Sierra Leone; isolated cases and small clusters in Senegal, Nigeria, U.S., and Spain (medical evacuations only in France, Germany, Norway, and UK) |
The animations below show the progression of the Ebola outbreak in West Africa. Outside of this region, Spain and the United States are the only countries with confirmed transmission of the virus. In both countries, secondary cases to date have occurred in healthcare workers who recently treated Ebola patients.
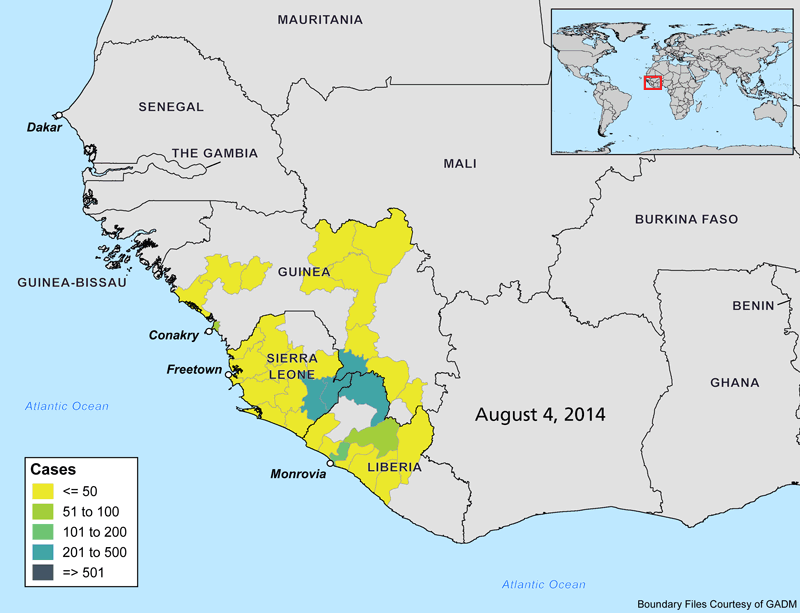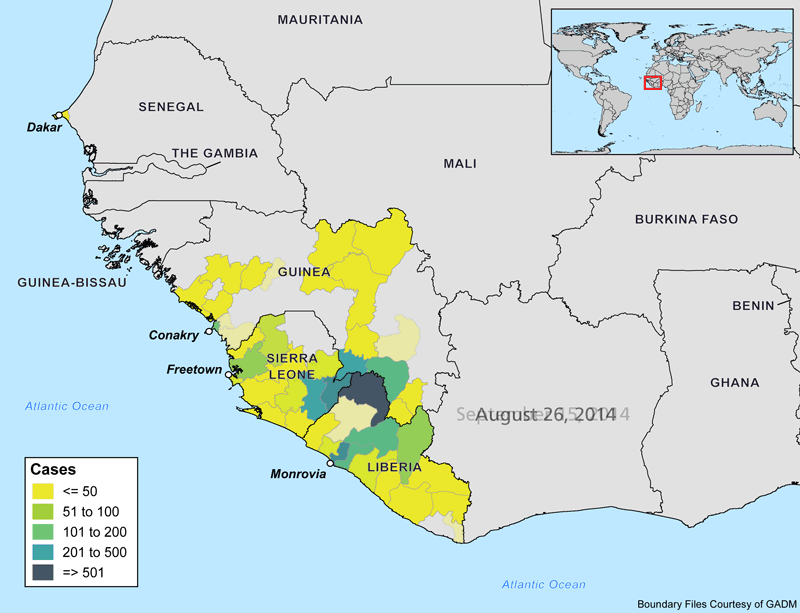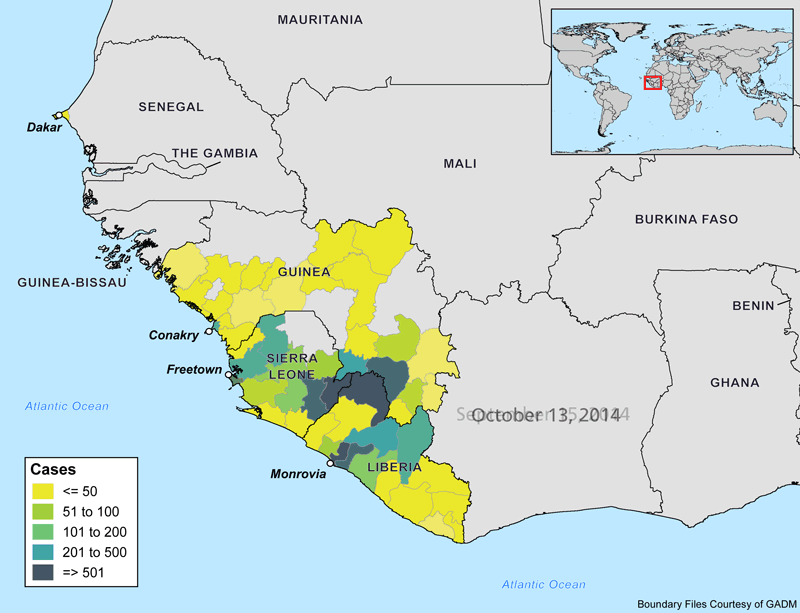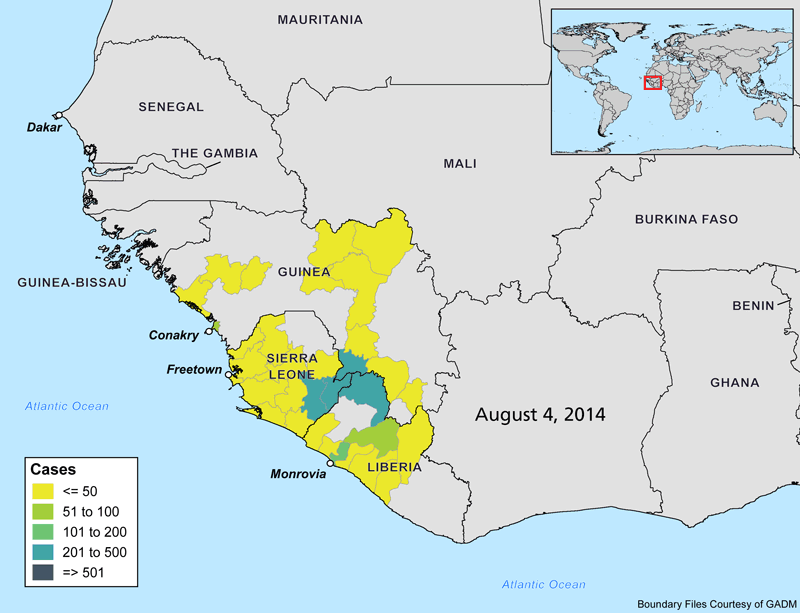
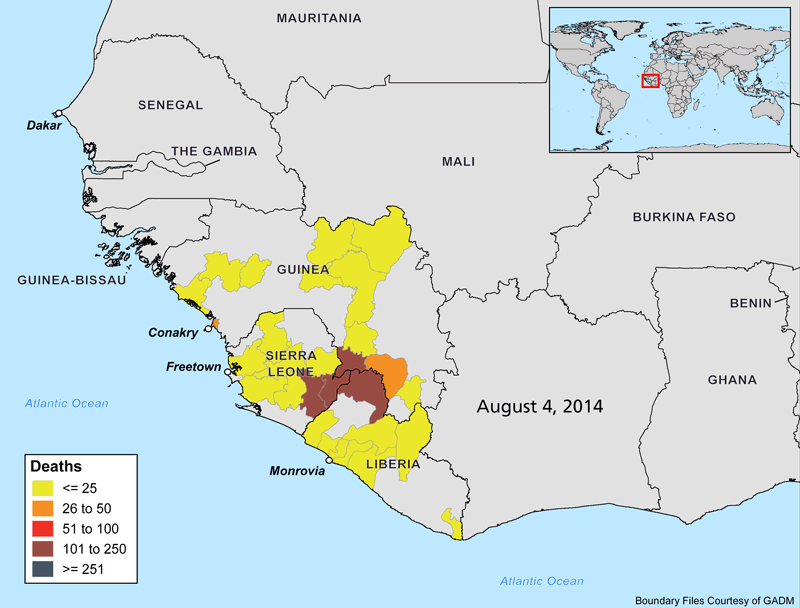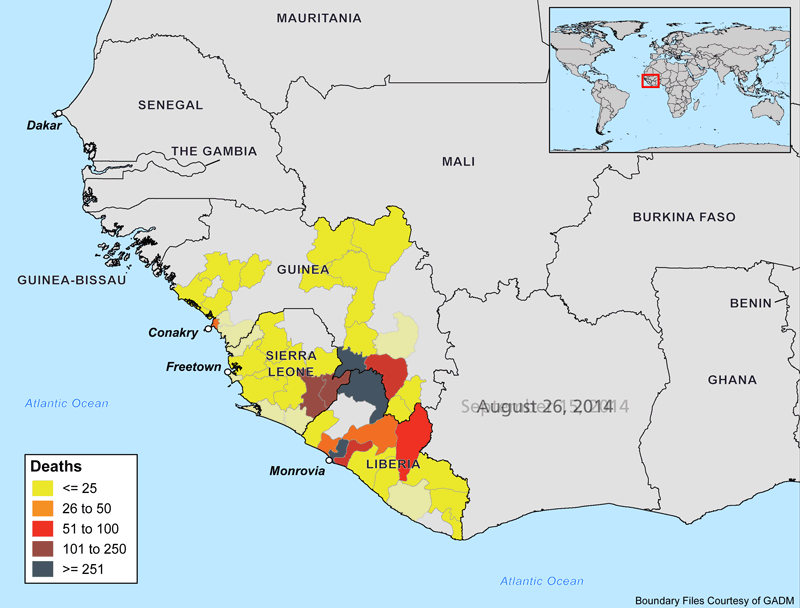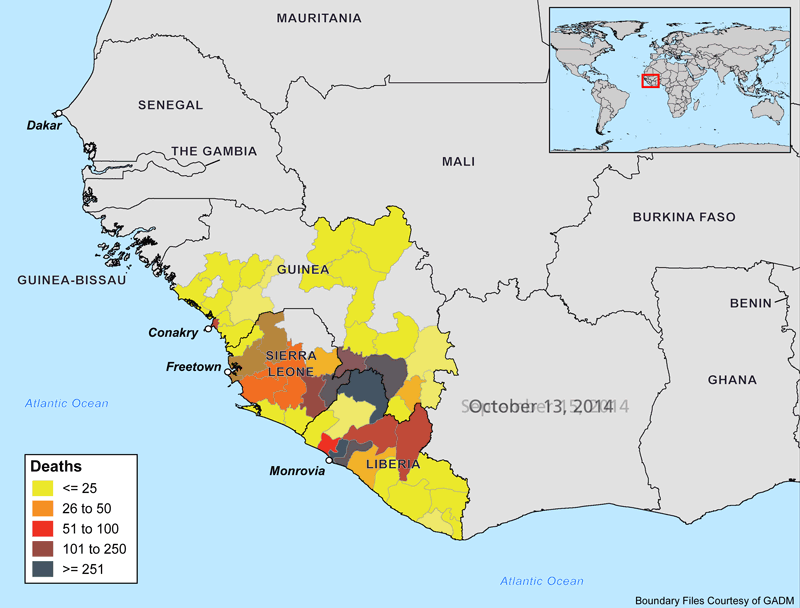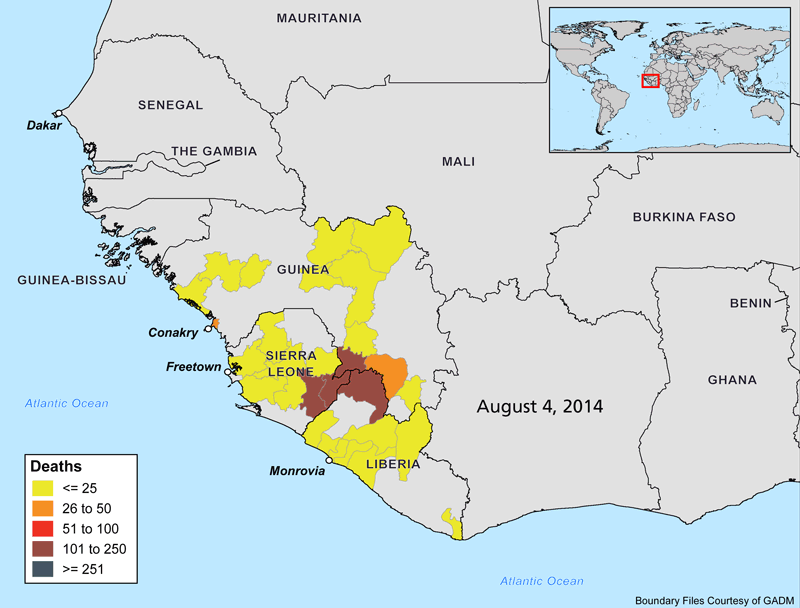
Why Is this Outbreak So Severe?
Initial estimates of virus-specific parameters—such as transmissibility and virulence (see callout box)—for the current outbreak are similar to the averages from 35 previous Ebola and Marburg outbreaks. So what is causing the unprecedented size and severity of this outbreak?
Changes in environmental and socio-economic factors may be to blame. These include urban transmission, population mobility, and inadequacy of healthcare infrastructure. This outbreak represents the first time intense virus transmission has occurred in very dense urban areas. In addition, this region of Africa has very porous international borders, and frequent population movement. Previous outbreaks have generally occurred in less populous, more isolated areas, where the ill and exposed could be more easily monitored and the outbreak could be more easily contained.
A second major factor in the explosive spread of this outbreak is the sorely lacking healthcare infrastructure of affected countries. Even before the outbreak started, Liberia and Sierra Leone had only about one doctor for every 100,000 people in a total population of about 10 million people. This is ten times lower than other African countries where previous Ebola outbreaks have occurred, and 200 to 400 times lower than most industrialized countries. In addition, many hospitals in the affected region lack basics, such as running water, soap, and gloves, let alone more specialized protective equipment, such as the goggles, masks, and gowns, that are typically required for working with Ebola patients. Further contributing to the spread of the disease, an estimated 10% of the infected are healthcare workers according to the WHO, which severely impacts the ability to fight the disease in three ways: first, it reduces the number of available healthcare workers and first responders; second, it may force some hospitals and wards to close due to lack of staff; third, it increases fear.
Another major issue is the mistrust between local populations and their governments. The skepticism has led to noncompliance, hiding sick people, attacks on medical workers, and "freeing" patients from treatment centers. This has put significant strain on the local and international communities trying to combat the problem.
Will Ebola Become a Global Pandemic?
The projections of the continued (and accelerating) spread of the virus are sobering. Estimates from various sources have indicated that without effective intervention, the global case count could reach 20,000 by early November (WHO), 200,000 by the year's end (Virginia Tech), and as many as 500,000 by the end of January 2015 (CDC), with the vast majority of cases limited to West Africa. (Note that models used by these different sources may have material differences in assumptions and methods.)
Of course, there is a high level of uncertainty associated with estimating the dynamics of a disease during an on-going outbreak. Preliminary estimates from AIR's soon-to-be-released Emerging Infectious Disease Model (which will be part of the updated AIR Pandemic Model) suggest that the projected outbreak sizes reported by these various groups are possible, especially if mitigation and containment measures in West Africa are not expanded.
While containing the current outbreak has proven difficult, the risk of sustained and widespread infection across multiple continents remains low. Scientists have used simulations of travel by airplane and local disease transmission dynamics to estimate the probability that an individual infected with Ebola will enter a foreign country undetected, and the expected number of people who would subsequently be infected. Their estimates show the likelihood of an Ebola-infected airline traveler arriving before the end of October is about 10%-20% for the United States, United Kingdom, France, and Belgium (since the U.S. has already had one imported case, this probability refers to the arrival of a second case). In fact, in any country with a robust healthcare system, any imported cases would most likely be contained with few (or no) transmissions to additional people—provided that cases are rapidly identified and appropriate infection control protocols are followed.
And finally, it is important to note that unlike influenza, which can be spread by small airborne droplets, Ebola is only spread by direct contact with bodily fluids. While some media outlets are warning of the possibility that the Ebola virus will mutate to become airborne, the WHO has stated that this is highly unlikely. Another difference between Ebola and the flu is that the flu can be transmitted before someone shows symptoms. Because Ebola is not airborne and can be transmitted only after symptoms appear, direct contacts of known cases can be identified, monitored, and treated, if needed, which allows for more successful containment.
Impact on the Insurance Industry
The Ebola outbreak in West Africa has taken a toll on the already fragile economies in the region. According to a recent analysis by the World Bank, short-term economic growth in Guinea, Liberia, and Sierra Leone may be severely impacted. If the outbreak continues through next year, the most severe scenario shows more than USD 30 billion in lost economic output in West Africa from 2014–2015. The World Bank noted that potential losses would be driven more out of "fear of contagion" than a direct result of the outbreak. Such an outcome could adversely affect insurance firms holding assets of companies with strong ties to West Africa.
In terms of direct losses resulting from insurance claims, widespread transmission in areas with a robust healthcare infrastructure can result in a spike in health insurance, life insurance, workers' compensation, travel insurance, and contingent business interruption claims. Insurance firms at highest risk are smaller niche insurance firms whose insurance pool may have a disproportionate impact relative to their competition or the larger insurance market.
However, widespread transmission in countries with a robust healthcare infrastructure and high insurance adoption is unlikely. A more likely scenario is a small number of cases arriving in theses countries from foreign affected areas. Individual cases could potentially lead to small, localized chains of transmission that would be contained by a swift response. These transmission chains are expected to be concentrated within first responders, healthcare workers, and family household clusters in highly localized areas. Insurance firms that have strong regional market share and family insurance plans in the regions most affected would likely incur the most insurance losses. Health insurance firms are anticipated to take the brunt of the effects. Life insurance firms may also be subject to smaller-scale concentration risk. In addition, workers' compensation claims are a distinct possibility among those who experience Ebola exposure on the job.
Few reports of direct healthcare costs are available. Costs for the first confirmed case in the United States (probably not covered by the commercial health insurance industry) are estimated to be nearly USD 500,000, reflecting the significant protective measures taken by healthcare professionals. For other people in the United States who contract the virus, costs will vary and will be influenced by a number of factors, most notably the length of hospital stay.
Costs for international health plans will also likely be very different and may include additional costs for medical evacuations. Several infected persons have been flown out of West Africa to hospitals, wards and medical treatment facilities that are better equipped and prepared to handle a patient with Ebola. Medical evacuations for this type of event are very complicated and present significant costs to the patient and insurance company. Medical evacuation is typically included in international health insurance policies, and could cost upwards of USD 100,000 per evacuation from West Africa. However, there may be coverage exclusions for medical evacuation during an epidemic, and several international medical insurance providers have stated that they will not cover the associated costs.
The loss from contingent business interruption and travel insurance is harder to assess and is highly impacted by a community's response and level of fear. Business interruption is most likely to occur in the mining, agricultural, energy, chocolate, and travel sectors. However, it is unclear what, if any, of these losses are covered by existing insurance policies, especially since business interruption policies typically require physical damage to a location. Basic travel insurance often only provides coverage in the event of weather, worker layoffs, or death of a travel companion. Some forms of travel insurance allow the covered party to cancel for any reason, though these are typically significantly more expensive.
In Closing
The Ebola outbreak has devastated families, healthcare systems, government institutions, and the local economies of the three worst-affected West African countries. According to WHO, "a coordinated international response is deemed essential to stop and reverse the international spread of Ebola."
In response to this call to action, many governments and non-government organizations have provided support for fighting this disease. This aid has come in many different forms, including sending healthcare workers, body disposal teams, medical testing kits, and supply kits to affected areas, and training response personnel. However, WHO has indicated that the current response is not adequate for containing the epidemic.
In mid October, WHO declared Senegal and Nigeria to be Ebola-free, after 42 days elapsed since the last cases were identified. However, for other affected countries, current estimates suggest that even with a significant uptick in containment measures, it may be another three to six months before the epidemic can be completely contained. It is still unknown what the final impact will be, but indications at present suggest limited direct impact to the global insurance industry. AIR will continue to closely monitor the situation. An in-depth Issue Brief is planned for release in the coming months that will contain modeled scenarios of the outbreak based on AIR's upcoming Emerging Infectious Disease Model, which will be part of the AIR Pandemic Model.
 By: Nita Madhav, MSPH, CCM
By: Nita Madhav, MSPH, CCM By: Doug Fullam, ASA
By: Doug Fullam, ASA By: Kierste Miller, MPH, CCM
By: Kierste Miller, MPH, CCM