In today's highly interconnected world, infectious diseases can spread rapidly and potentially cause catastrophic losses. With its capabilities for efficient transmission and elevated virulence, influenza is believed to have the greatest pandemic potential of known infectious diseases. In addition to affecting a variety of people and places, a wide array of business sectors can be impacted when an outbreak strikes.
AIR has created a tool to quantify the potential losses associated with private health insurance claims during outbreaks to more explicitly capture the risk associated with this line of business. This healthcare use module takes a probabilistic approach to create a comprehensive view of inpatient, outpatient, and prescription costs during outbreaks.
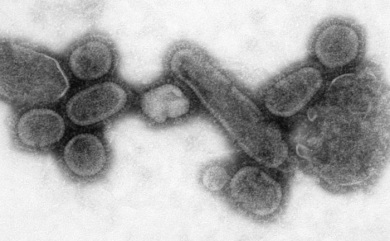
(Source: Centers for Disease Control, Dr. Terrence Tumpey, Cynthia Goldsmith)
Because the potential virulence of pandemic influenza varies considerably between strains, it is useful to consider a range of plausible scenarios for the next flu pandemic. For example, one pathogen may cause relatively few fatalities and hospitalizations but result in numerous clinic visits, which can aggregate to a high total cost. Another strain of flu, however, may cause an unusually high number of hospitalizations or deaths in a particular age group.
On average, about 200,000 hospitalizations occur every year in the United States alone due to flu-related heart and respiratory conditions, and millions seek care for flu infection from outpatient clinicians. Imagine how significantly these values may escalate during a large-scale flu pandemic.
In the AIR healthcare utilization module, location- and age-specific severity functions estimate the number of infections that result in outpatient and inpatient care during each simulated event. Modeled healthcare use is correlated to local resource availability, including hospitals and doctors per capita, around the world. These counts can then be translated into financial terms using either AIR-provided industry average benefit values or user-defined benefit levels.
The 1918 "Spanish Flu" pandemic was one of the largest public health catastrophes in modern history. Caused by a readily transmissible and highly virulent strain of influenza, the event killed somewhere between 20–100 million people worldwide, at a time when the global population totaled just 1.8 billion. Fortunately, the world is far better prepared to face outbreaks of disease today than it was in 1918.
Scientific advancements and global cooperation allow for better and more rapid response to widespread illness. This does not, however, guarantee that a pandemic could not happen today. Our aging population could be far more susceptible to disease, resistant strains of pathogens are being discovered more frequently, the human response is unpredictable, rate of infection is uncertain due to global interconnectivity, our changing climate could impact disease growth and spread, and shifting animal habitats may expose humanity to more and new illnesses.
While the superior health care that we now have may help us mitigate a catastrophe, that care is generally more expensive today than the care that was available during historical pandemics after correcting for the effects of inflation. This factor increases the potential healthcare-related costs during future pandemics.
Modeling strategies elucidate the potential impact of events similar to the historical "Spanish Flu," along with the wide range of scientifically plausible pandemics, if they occurred in the modern healthcare setting. With these AIR modeling tools, you can formulate a robust view of risk associated with healthcare use and mortality during infectious disease events.